Abstract
Introduction: Sinusoidal obstruction syndrome (SOS) is a disease which is caused by toxic injury to hepatic sinusoids. This syndrome is most frequently caused by myeloablative radiochemotherapy in patients before hematopoietic stem cells transplantation and also by oxaliplatin mainly in patients with colorectal liver metastases. The aim of this study was to establish a large animal model of SOS, which would enable further study of this disease and facilitate translation of experimental outcomes into human medicine.
Methods: A total of 27 domestic pigs (Prestice Black-Pied pig) were involved in this study (12 females). A group with a higher dose of monocrotaline (180 mg/kg) included 5 animals, and the remaining 22 pigs formed another group with a lower dose (36 mg/kg). Monocrotaline was administered via the portal vein and one week after the administration, partial hepatectomy of the left lateral liver lobe was performed. The animals were followed up for 3 weeks after monocrotaline administration. Regular ultrasound examinations were performed as well as examination of biochemical markers of liver and kidney functions and histological examination of liver parenchyma samples.
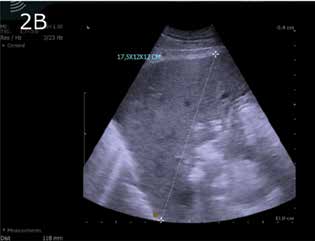
Results: The features of toxic liver injury which we observed in case of all animals were comparable with macroscopic and microscopic appearance of SOS. We recorded AST, ALT, bilirubin and ammonia elevation after monocrotaline administration. Echogenicity on ultrasound images of injured liver parenchyma was higher compared to echogenicity of healthy parenchyma. All the five animals from the first group with a higher monocrotaline dose had died before partial hepatectomy (1st–3rd day after monocrotaline administration). Death before partial hepatectomy occurred in 3 cases (6th and 7th day after monocrotaline administration) in the second group of 22 animals with a lower dose of monocrotaline. Death after partial hepatectomy occurred in 8 cases (7th–17th day after moncrotaline administration) in the same group. 11 animals survived the entire experimental period. The cause of death (in both groups) was metabolic failure in 10 animals and exsanguination in 4 animals, both due to severe hepatopathy. Death of 2 animals was not associated with monocrotaline intoxication (strangulation of small intestine, gastrectasis).
Conclusions: We established a large animal model of SOS induced by monocrotaline administration (36 mg/kg via portal vein). This model can contribute to research of therapeutic modalities for this disease or to evaluation of surgical treatment of patients with SOS.