Abstract
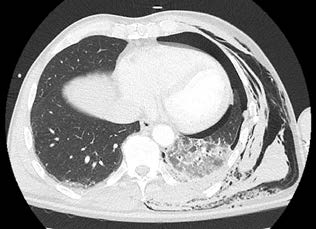
Pulmonary contusion is a common finding after blunt chest trauma. It occurs in 23–35% of all cases. Alveolar capillaries are injured due to the trauma, which results in accumulation of blood and other fluids within lung tissue. The fluids interfere with gas exchange, leading to hypoxemia. The consequences of pulmonary contusion include ventilation/perfusion mismatching, increased AV shunts and loss of compliance of lung parenchyma. These physiological consequences are manifested within hours from injury and usually resolve in 7 days. Computed tomography (CT) is a sensitive and main diagnostic tool. Clinical symptoms include hypoxemia and hypercapnia, manifested predominantly during 72 hours from injury. Patients are treated primarily conservatively; surgery may be needed due to haemothorax associated with lung contusion or progression of AV shunts due to localized pulmonary contusion.